Gliomas are one of the most common types of brain tumors – and one of the most difficult to treat. Surgery to remove the tumor, usually the first treatment step, is complicated because gliomas don’t have clear biological boundaries. They are surrounded by what’s similar to a fog.
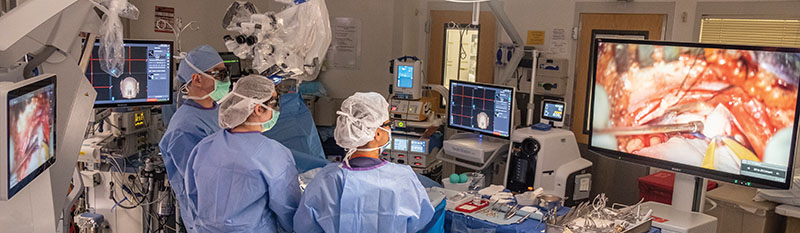
Using revolutionary, game-changing technology – along with 3D glasses, high-definition monitors and a robotic exoscope – the entire surgical team can now see the minute inner workings of the brain with pinpoint accuracy
Did You Know?
50% of patients
treated at the Gerald J. Glasser Brain Tumor Center are battling gliomas.

“Glioma surgery entails sculpting out a tumor that truly cannot be seen because of the surrounding fog and its relative positioning to the brain,” explains Yaron A. Moshel, MD, PhD, Co-Director of the Gerald J. Glasser Brain Tumor Center.
“When these dense tumors infiltrate the body’s most complicated organ, the brain, and become intertwined with the functional areas that control language, memory, motor and sensory skills – as they often do – the risks and challenges of removing them intensify.”
Removing gliomas as safely and completely as possible requires years of experience and a deep understanding of the brain’s three-dimensional anatomy and functional relationships. Today, this expertise is supported by technological advances that enable more precise, less invasive tumor removal.
From 2D to 3D with Stereotactic Guidance
Traditionally, neurosurgeons used two-dimensional MRI scans taken before surgery to help them envision the tumor and guide their approach in the operating room. Now, with Medtronic’s Stealth Station S8 Surgical Navigation System – the most advanced stereotactic guidance available – multiple types of MRI scans, including functional scans that illuminate speech and motor centers, can be overlaid with three-dimensional images of the tumor. This imaging and GPS-like technology help identify the tumor’s boundaries and provide a precise surgical line of sight.
“The move from 2D to 3D is significant,” adds Fabio Frisoli, MD, a neurosurgeon at the Glasser Center. “With a 3D view of the tumor, you’re much more likely to be able to remove the tumor in its entirety while minimizing any potential disturbance to other areas of the brain.”
Fluorescent Imaging, Glowing Tumors and the Standard of Care for the Future
Fluorescent imaging is one of the newest advancements in brain tumor care. Patients ingest 5 ALA, a liquid solution that circulates throughout the body and causes a malignant tumor to glow a bright orange color. The tumor fluorescence is seen with a special microscope equipped with a highly specific blue light filter. After years of use abroad, this emergent technology was recently approved for use in the US.
“The Glasser Center is one of the first providers in New Jersey to harness the power of fluorescent imaging for brain tumor care. We believe this fluorescent tracer will become the standard of care because of the immense advantage it provides in distinguishing malignant cells from healthy tissue,” says Dr. Moshel.
Combining Technologies with Advanced Microscopes
The newest microscope, the Zeiss Kinevo, incorporates intraoperative fluorescent imaging of the tumor and the Stealth Navigation 3D images, giving neurosurgeons every piece of information they need during surgery, including a “heads-up display.”
“Before this technology, neurosurgeons would essentially look at a screen on their left displaying an MRI, then turn back to the operating table to apply what they saw on screen to the patient in front of them,” explains Dr. Moshel. “This combination of technologies now allows us to see everything right in front of us and safely remove some of the most complex tumors in some of the most difficult-to-reach locations.”
Getting it Right the First Time
When it comes to gliomas, removing the tumor in its entirety – versus one piece at a time – is particularly important. Advanced technology makes this possible, allowing neurosurgeons to more easily follow the outer wall of the tumor and dissect around it, like peeling an orange.
If the entire tumor is not removed and a patient begins follow-up radiation, the residual tumor can swell, ultimately requiring the patient to stop treatment and undergo a second surgery. At the Glasser Center, we have seen this in patients who have come to us for help after initial surgeries performed elsewhere. Factoring in post-op recovery time before resuming treatment, this can easily set a patient back by two months or more. This not only impacts survival rates, but can also alter a patient’s course of treatment.
Request More Information
Please use the form to request more information.
All fields are required.
Please note that this form is for North American residents only.