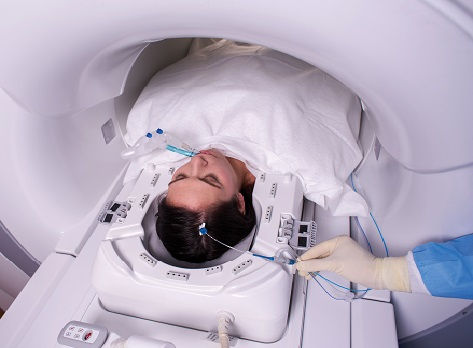
Treatment for brain cancer and epilepsy has reached a remarkable milestone with the advent of laser interstitial thermal therapy (LITT), providing patients with a minimally invasive surgical option for recurrent brain tumors, radiation necrosis and certain types of epilepsy.
Neurosurgeons performing LITT use magnetic resonance imaging (MRI) to guide a small probe with a laser that delivers precisely controlled heat to destroy unhealthy brain and cancer tissue. Also known as laser ablation, this innovative technique allows patients who previously would have undergone more invasive surgical procedures, accompanied with longer recovery time, to instead experience shorter hospital stays and lower risk of complications.
A New Alternative to Open Surgery
“LITT provides a major advantage for our patients and is an important tool in our ever-expanding toolbox” says Yaron Moshel, MD, a fellowship-trained neurosurgeon and co-director of Gerald J. Glasser Brain Tumor Center at Atlantic Health System. “Our multidisciplinary team of experts are adept at finding the most effective treatment options and we are proud to offer this cutting-edge technology.”
Until recently, many patients with gliomas, brain metastases, radiation necrosis and some forms of epilepsy required traditional open skull surgery, called a craniotomy, to remove tumors and epileptic foci. This type of surgery can require a hospital stay, recovery time, rehabilitation, and physical therapy. Patients battling cancer with chemotherapy often need to pause treatment to prepare for open surgery, losing precious time.
By contrast, LITT is minimally disruptive to the brain and is suitable for most patients, even those on chemotherapy who are not candidates for open surgery. During LITT, a neurosurgeon opens a very tiny hole in the skull while the patient is asleep under anesthesia. Then, using stereotactic guidance (a GPS system for the brain based on an MRI scan), and sometimes, a robotic arm, the surgeon places a thin fiberoptic probe within the area of the brain that is the focus of treatment. Once it is in place, the remainder of the procedure is completed in an MRI machine, where a laser beam travels through the probe to thermally treat the tumor. The body’s natural immune system then cleans up the debris left behind after the thermally treated tumor cells disintegrate.
The Power of Laser Technology
“Most people think of a laser as something from “Star Wars”. In fact, a laser is an extraordinarily precise device, that with proper monitoring, can direct controlled heat inside a tumor, destroying malignant cells without damaging the healthy tissue that surrounds it,” explains Dr. Moshel.
While the heat from the laser is being deployed within a tumor, or, in the case of treating epilepsy, creates a lesion in the region of the brain that is causing seizures, the neurosurgeon uses MRI as a 3-D thermometer to determine how far the heat has spread and to verify the efficacy of the procedure. The heating and cooling of the laser is regulated automatically to prevent damage to healthy tissue surrounding the unhealthy tissue. The MRI provides live imaging and feedback in real time. At the conclusion of the procedure, the neurosurgeon removes the probe and, if necessary, seals the tiny incision.
The Benefits of LITT
“A clear advantage of LITT is that patients are spared the physical stress and recovery times of open surgery. In fact, because the incision is so small, the patient often requires little to no recovery time,” says Dr. Moshel. “Usually, stitches are not even needed at the site of the incision. Many patients go home either the day of the procedure or the next day.”
Once an emerging procedure, LITT technology is rapidly becoming standard practice and an accepted adjunct to surgery and radiation therapy. At the Brain Tumor Center, a multidisciplinary team of neuro-oncologists, neurosurgeons, radiation oncologists, epileptologists and other specialists determines a patient’s eligibility and recommends the most effective course of action for each individual, based on their specific needs.
“We have designed a program that puts patients and families at the center of everything, with the nation’s top medical experts, the latest minimally invasive and image-guided neurosurgical techniques. Here, patients and their loved ones navigate the journey from diagnosis through treatment. Throughout each step, they are surrounded by the support and guidance of a multidisciplinary team of experts who deliver state-of-the-art care with state-of-the-art compassion” says Dr. Moshel.
Clinical innovation has always been a hallmark of the work performed at Gerald J. Glasser Brain Tumor Center and LITT is simply the latest advancement that provides patients with the most effective treatment options, including other noninvasive approaches such as CyberKnife® radiosurgery. Each year, more than a thousand families turn to us to care for their loved ones. The Atlantic Neuroscience Institute has been ranked first for neurosurgery in NY, NJ, CT and PA, and is among the top 5% of the nation’s neuroscience programs five years in a row.
Individualized Care for Brain Tumors
Our specialists hold your hand each step of the way through comprehensive brain tumor care that integrates science, innovation and expertise.