Brain Tumor Treatment Options
At the Gerald J. Glasser Brain Tumor Center, part of Atlantic Health System Neuroscience and Atlantic Health System Cancer Care, we treat brain tumors using individualized treatment plans that incorporate some of the safest and most advanced techniques available.
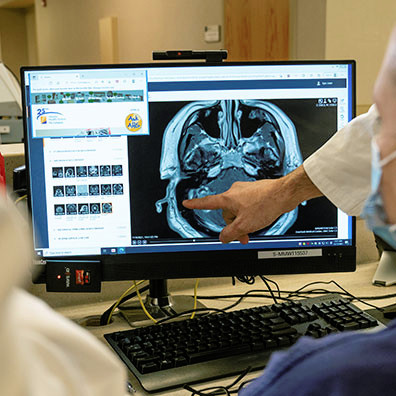
Advanced Techniques
The expertise of our clinical staff is constantly growing. Cutting-edge technologies and techniques we use include CyberKnife, conformal radiation, brain mapping and awake surgery, image-guided stereotactic volumetric craniotomy, fluorescent imaging, minimally invasive endoscopic brain surgery, and more.
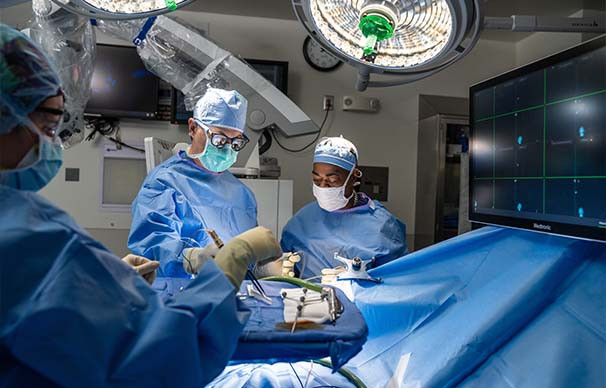
Treatment and Expertise
Our deep expertise in brain tumor care spans a wide array of novel treatments and therapies that help deliver the best possible outcomes to our patients. Treatments include:
Stereotactic Radiosurgery (CyberKnife®)
We use precise, high-dose radiation with pinpoint accuracy to target cancerous and non-cancerous tumors without damaging surrounding healthy tissue. Radiosurgery is a non-invasive and painless treatment in which robotic technology is used to deliver pinpoint beams of highly focused radiation. This form of focused radiation has improved the quality of life for many of our patients with brain tumors. We use CyberKnife, at Overlook Medical Center, and TrueBeam, at Morristown Medical Center, to treat patients closest to home and based on their specific diagnosis.
Minimally Invasive Craniotomy
Neurosurgeons use specialized tools to temporarily remove part of the bone of the skull to access a brain tumor. We use the latest techniques and technology – like stereotactic 3D image guidance, high-powered robotic microscopes, fluorescent imaging, 3D volumetric techniques and more – to make this procedure as safe and effective as possible. These advanced visualization techniques enable our surgeons to use smaller incisions during surgery.
3D Stereotactic Image-Guided Surgery
A computer system in the operating room helps our neurosurgeons achieve pinpoint accuracy. The system combines MRI-based imaging as well as other functional imaging and brain connectivity information into a 3D model of the patient’s brain. Our neurosurgeons can use this model – much like a map and GPS device – to safely remove as much of the tumor as possible and to calculate safe pathways to deep-seated tumors that are otherwise considered inoperable.
Functional Brain Mapping and Awake Surgery
We use functional brain mapping when tumors or neurological conditions occur near important movement, sensory and language centers of the brain that are unique to each patient. Our neurosurgeons and their team of neurophysiologists use electrical stimulation to interactively map these functional areas during surgery while the patient is awake and under the care of a specialized anesthesiologist. Speech and motor functions are monitored and preserved while as much of the tumor as possible is removed.
Minimally Invasive Endoscopic Brain Tumor Surgery
Using stereotactic image guidance and a small fiberoptic camera called an endoscope, neurosurgeons can safely remove tumors deep within the brain, ventricles and skull base, including the pituitary gland. They do this with great accuracy through small, minimally invasive incisions or by simply going through the nose. A team of specialists, which may include an otolaryngologist (ENT) and a neurosurgeon, usually performs these procedures together.
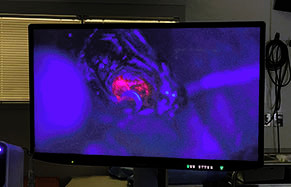
Surgery Guided by Fluorescent Imaging
Our team is one of the few in New Jersey to harness the power of fluorescent imaging, a groundbreaking technology. After drinking a liquid solution, a patient’s cancerous tumor glows a pink fluorescent color. Using a special microscope and filter, our surgeons can distinguish the cancer cells from healthy brain tissue for precise removal of the tumor.
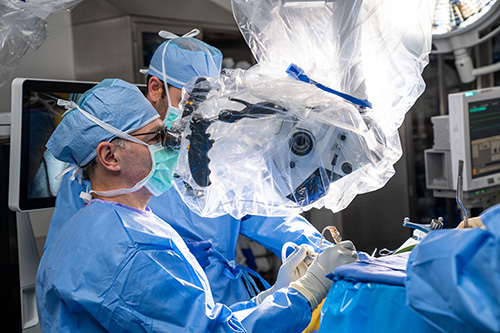
Skull Base Microsurgery
Open skull base surgery has become safer and more effective because of advanced surgical techniques that use high-powered magnification. In this surgery, the bone at the bottom of the skull is removed to access hard-to-reach tumors. In some cases, minimally invasive techniques and endoscopy are also used. A multi-disciplinary team of specialists plans the surgery and follow-up treatments. A team of neurophysiologists assists during the procedure to ensure critical brain and delicate nerve functions are monitored and preserved.
Laser Interstitial Thermal Therapy (LITT)
A minimally invasive surgical alternative to open craniotomy. LITT may benefit patients with brain tumors, radiation necrosis, or medically refractory focal epilepsy. While the patient is asleep under anesthesia, the surgeon creates a small hole in the skull. Using MRI and robotic guidance, the surgeon navigates a fiberoptic wire toward the tumor. Once the fiberoptic wire is in place, a laser is used to thermally destroy the tumor or create a lesion. The procedure is completed in the MRI suite where the thermal damage to the tumor is visualized in real time. The surgeon then removes the wire and closes the incision.
Embolization
Using a minimally-invasive embolization procedure, our endovascular neurosurgeons can shut down the blood flow to a tumor in preparation for surgery. This causes the tumor to shrink, makes removal easier and reduces risks of bleeding and nerve damage during surgery.
Neuro-Oncology
Experts in both neurology and oncology, our neuro-oncologists specialize in treating cancers that start in – or spread to – the brain and central nervous system. With a robust clinical trial and research portfolio, they deliver extraordinary brain tumor care and treatment for the neurological complications of cancer. We work closely with each patient’s medical oncologist to maximize quality of life. This includes helping manage the headaches, strokes, seizures and nerve problems (peripheral neuropathy) that may arise from chemotherapy or cancer itself.
Targeted Therapy
New treatments for brain tumors – such as drugs that target a specific mutation found in a subset of tumors – are proposed every year. We use each patient’s brain tumor molecular profile – a unique map of all the mutations within their brain tumor – as a guide to determine which potential cutting-edge therapy may be effective. These profiles also drive our understanding of tumor behavior and treatment, help us identify mutations that do not yet have treatments, and inform future studies and the development of new drugs.
Immunotherapy
Immunotherapy uses the body’s own immune system to fight cancer cells as if they are an infection. Having already shown impressive results in other cancers, the use of immunotherapies in brain tumor treatment is growing. Our team offers immunotherapy treatments to our patients and explores ways to further harness this technology.
Tumor-Treating Fields
Tumor-treating fields (TTFields) therapy uses alternating electromagnetic fields to disrupt cancer cell division. These fields are delivered through ultrasound and act regionally and non-invasively to inhibit tumor growth. TTFields therapy is U.S. Food and Drug Administration approved for the treatment of glioblastoma multiforme, the most common and aggressive brain cancer. Studies demonstrate improvement in overall survival when added to standard therapies.
Chemotherapy
New advances are opening the door to novel chemotherapy treatments. These include the use of molecular information about individual patients’ tumors to determine the best chemotherapy regimen, new medications that block the growth of resistant cancer cells, new combinations of therapies and immunotherapy that stimulates a patient’s own immune system to selectively attack cancer cells.
Image-Guided Conformal Radiation
This type of radiation therapy uses imaging scans to accurately deliver high-energy beams of radiation to a narrowly focused area of the brain or skull base. With the help of our physicists and radiation oncologists, imaging scans are conducted prior to each treatment and the patient’s position is monitored throughout the radiation treatment.
Neuropathology and Molecular Diagnostics
Our neuropathologists specialize in microscopic tissue examination and the emerging field of molecular diagnostics. By studying the unique genetic profile of each tumor using modern, gene-chip technology, we can determine genetic mutations faster than ever before. This empowers us to design tailored, targeted treatments based on each tumor’s DNA. We are one of the only centers with these specialists.
Brain Tumor Diagnostic Tests and Screenings
At the Glasser Brain Tumor Center, part of Atlantic Neuroscience Institute and Carol G. Simon Cancer Center, we know that the timely, accurate diagnosis of brain tumors is vital to improving outcomes. Tests that we use to diagnose tumors include:
- Magnetic resonance imaging (MRI) with diffusion and perfusion imaging
- Functional MRI
- Diffusion tensor imaging (DTI)
- Stereotactic image-guided brain biopsy
- Neuropathology and tumor subtyping
- Molecular testing